PCOS: A Holistic Approach to Hormonal Health in Women
Apr 20, 2026
Polycystic Ovary Syndrome (PCOS) is one of the most commonly diagnosed hormonal conditions in women, yet for many, the experience of living with it feels anything but clear or straightforward. It often begins with almost unnoticeable subtle changes in cycle, energy, skin, or weight, and over time becomes something that feels harder to ignore, yet not always fully explained.
In modern healthcare, PCOS is typically approached as a reproductive or endocrine disorder. And while this is true, it is only part of the picture. When we look more closely, PCOS reveals itself as a broader pattern within the body, one that involves metabolism, the nervous system, and the way the body responds to stress, nourishment, and daily life.
Understanding this opens the door to a more complete and practical way of working with it.
What is PCOS?
PCOS is a hormonal condition characterised by irregular ovulation, elevated levels of androgens (such as testosterone), and changes in ovarian function. Despite the name, the presence of cysts is not required for diagnosis, and many women with PCOS may never develop them.
What defines the condition more accurately is a disruption in hormonal communication. The brain, through the hypothalamus and pituitary gland, sends signals to the ovaries to regulate ovulation. In PCOS, this communication becomes altered, often leading to increased androgen production and irregular or absent cycles.
Alongside this, many women experience insulin resistance, where the body’s cells become less responsive to insulin. This results in higher circulating insulin levels, which further stimulates androgen production and contributes to the cycle of hormonal imbalance.
Rather than being isolated to the ovaries, PCOS is better understood as a condition involving the entire endocrine and metabolic system.
How Common is PCOS?
PCOS affects a significant portion of the female population, with estimates suggesting around one in eight to one in ten women are living with the condition. Despite this, a large number of cases remain undiagnosed, often because symptoms are normalised, dismissed, or managed individually rather than recognised as part of a pattern.
It is also one of the leading causes of infertility and is strongly associated with insulin resistance, even in women who appear otherwise healthy. Over time, if left unsupported, it may increase the risk of type 2 diabetes, cardiovascular conditions, and ongoing metabolic dysfunction.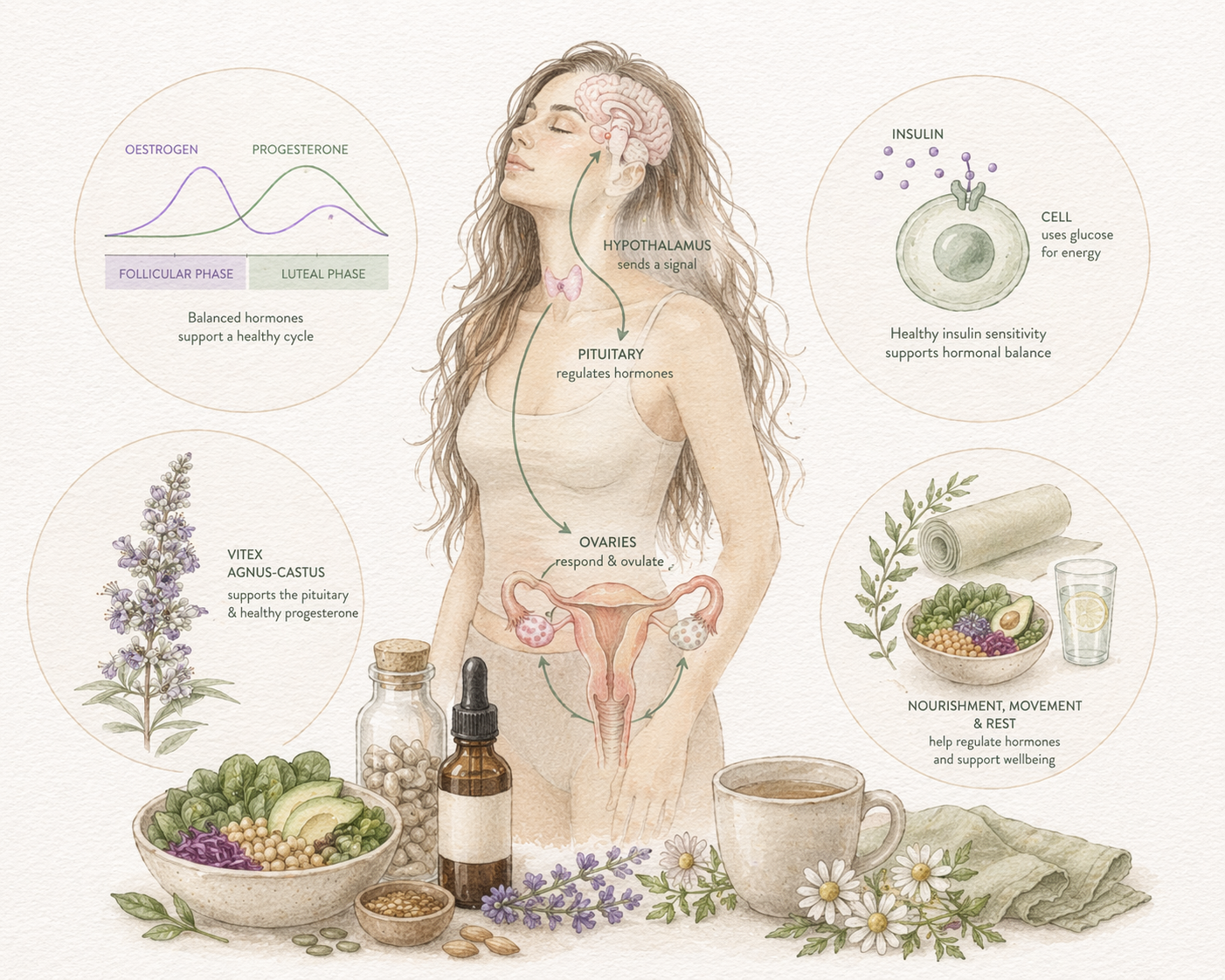
Signs and Symptoms of PCOS
The experience of PCOS can vary widely from woman to woman, which is part of what makes it difficult to identify early. For some, it presents primarily through irregular or absent menstrual cycles, while for others, it may show up as persistent acne, unwanted hair growth, or difficulty maintaining a stable weight. Many women describe a deeper layer of symptoms that are less visible such as fatigue that doesn’t quite lift, brain fog, fluctuating moods, or a sense that their body is working against them. These experiences reflect the underlying hormonal and metabolic shifts taking place, particularly around insulin regulation, androgen levels, and nervous system load.
Understanding the Pathogenesis
To understand PCOS more clearly, it helps to step back and look at the interplay between the body’s systems. At a hormonal level, the signalling between the brain and ovaries becomes dysregulated. Increased luteinising hormone (LH) stimulates the ovaries to produce more androgens, which can interfere with ovulation. At the same time, insulin resistance drives higher insulin levels, further amplifying androgen production.
Overlaying this is the influence of chronic stress. Elevated cortisol levels, disrupted sleep, and a consistently activated nervous system all contribute to metabolic strain and hormonal imbalance. Inflammation also plays a role, subtly reinforcing the cycle over time. What emerges is not a single issue, but a pattern: a system under pressure, adapting in ways that eventually become symptomatic.
A Common Medical Experience
For many women, the journey begins in a clinical setting. After noticing changes in their cycle, skin, or weight, they seek answers and are eventually diagnosed with PCOS through blood tests and/or ultrasound. The standard approach often includes prescribing the oral contraceptive pill or other hormonal treatments to regulate cycles and, in some cases, medication such as metformin to address insulin resistance. These interventions can be helpful, particularly in managing symptoms and reducing certain risks.
However, it is not uncommon for a woman to feel that while her symptoms are being managed (or masked!), her understanding of what is happening in her body remains limited. The deeper drivers like stress, lifestyle patterns, and metabolic health are not always explored in detail, leaving a gap between treatment and true resolution.
An Ayurvedic Perspective
From an Ayurvedic lens, PCOS is not seen as a fixed condition, but as an expression of imbalance within the body. There is often a combination of kapha qualities like heaviness, stagnation, accumulation; alongside vata disturbance, which brings irregularity and instability. Digestion, or agni, is frequently compromised, leading to the buildup of ama (metabolic waste), which can further obstruct the body’s natural processes.
Rather than focusing on the diagnosis itself, the approach becomes one of restoring rhythm. Regular meals, warm and nourishing foods, daily routines, and gentle detoxification practices begin to support the body in returning to balance. Over time, as digestion improves and the nervous system settles, many women notice their cycles becoming more regular and symptoms easing.
It is not a quick fix, but it is a steady and sustainable one that helps to treat the root cause, as opposed to the symptoms.
An Integrative Approach
Increasingly, women are choosing a more integrative path - one that draws from both modern medicine and holistic practice. In this approach, medical testing provides clarity around hormone levels and metabolic markers, while lifestyle and therapeutic practices address the underlying patterns. Medication may be used where appropriate, particularly in the early stages, but it is supported by changes in nutrition, movement, stress management, and daily rhythm. This creates a sense of partnership with the body rather than control over it. There is both structure and flexibility, and over time, many women find they are able to reduce their reliance on external interventions as their internal systems become more regulated.
Lifestyle Support for PCOS
The most impactful changes in PCOS tend to come through daily life through consistent, supportive habits that gradually shift the body’s internal environment.
Yoga-asanas can play a valuable role here, particularly when approached as a tool for regulation. Slower, grounding practices help to calm the nervous system, while breathwork techniques such as alternate nostril breathing or humming breath support hormonal balance indirectly through stress reduction. Gentle movement through the hips and abdomen encourages circulation, while deep rest practices allow the body to restore and recover.
Eating regularly, choosing whole and minimally processed foods, and combining protein, fats, and fibre in meals helps to regulate blood sugar and reduce insulin spikes. Warm, digestible meals support gut health and reduce the burden on digestion, which is often compromised in PCOS.
Herbal support can also be beneficial when used appropriately. Herbs such as ashwagandha for stress resilience, shatavari for reproductive support, and turmeric for inflammation are commonly used, though they are most effective when tailored to the individual. Vitex (Vitex agnus-castus) is often spoken about in relation to hormonal balance, and in some cases of PCOS it can be supportive, particularly where there is irregular ovulation or low progesterone. Rather than acting as a hormone itself, it works through the pituitary gland to support the body’s natural hormonal signalling. However, PCOS presents differently in each woman, and in cases where there are higher androgen levels or significant insulin resistance, Vitex may not be the most appropriate herb. It tends to be most effective when used within a broader, personalised plan that includes nutrition, lifestyle, and metabolic support, under the guidance of a suitable health practitioner.
Strength training and walking tend to support metabolic health without overstressing the system, while excessive high-intensity exercise can sometimes exacerbate hormonal disruption if the body is already under strain.
A Different Way of Seeing PCOS
PCOS is often framed as something to manage or control, but this perspective can feel limiting. When understood more broadly, it becomes clear that the body is not failing, it’s working hard ot adapt. The symptoms are signaling toward areas that need support. With the right approach, one that combines understanding with practical, daily action, PCOS becomes far less overwhelming. It becomes something that can be worked with as part of a larger process of returning the body to balance.